New Treatments for Fibromyalgia: What Actually Works in 2026
If you have fibromyalgia, you have probably been told some version of “we do not really know what causes it” followed by a prescription for medication that barely takes the edge off. I get it. The frustration of living with widespread pain that nobody can fully explain â and that many doctors still do not take seriously â is exhausting in a way that goes beyond the physical.
I have been working with acupressure and pain management since 2017, and fibromyalgia is one of the conditions I hear about most. The women and men who reach out to me are not looking for another pill. They want something that actually changes how their body feels day to day. And the good news is that the treatment landscape for fibromyalgia has shifted significantly in recent years. There are approaches that work â real, evidence-based strategies that go beyond “learn to live with it.”
This guide covers the newest and most effective treatments for fibromyalgia in 2026, from emerging medical therapies to the hands-on approaches that many people find more helpful than anything their doctor has prescribed.
What Is Fibromyalgia and Why Is It So Hard to Treat
Fibromyalgia is a chronic condition characterized by widespread musculoskeletal pain, fatigue, sleep disturbances, and cognitive difficulties often called “fibro fog.” It affects an estimated 2-4% of the global population, with women diagnosed roughly seven times more often than men.
The reason fibromyalgia is so difficult to treat is that it is not a problem with your muscles, joints, or tissues in the traditional sense. It is a central sensitization disorder â your nervous system has essentially turned up the volume on pain signals. Normal sensations that should not hurt become painful. Mildly uncomfortable stimuli become excruciating. And the pain moves around, which makes it even harder to pin down.
This is why treatments that target specific body parts often fail. You are not treating a damaged knee or a herniated disc. You are treating a nervous system that has lost its ability to properly regulate pain signals. The most effective treatments address this central mechanism directly.
Emerging Medical Treatments
The medical understanding of fibromyalgia has advanced considerably, and several newer treatment approaches show genuine promise.
Low-Dose Naltrexone (LDN)
Low-dose naltrexone has become one of the most talked-about emerging treatments for fibromyalgia, and the research is catching up to the anecdotal reports. At doses of 1.5 to 4.5 mg â far lower than the standard dose used for addiction â naltrexone appears to reduce neuroinflammation by modulating microglial cell activity in the central nervous system.
A 2023 systematic review published in Biomedicines found that LDN reduced fibromyalgia pain scores by an average of 30% compared to placebo. Patients also reported improvements in fatigue, sleep quality, and overall quality of life. Side effects were minimal â mainly vivid dreams in the first few weeks.
LDN is not yet FDA-approved specifically for fibromyalgia, which means your doctor may not bring it up. But it is available as an off-label prescription through compounding pharmacies. If your current treatment is not giving you adequate relief, it is worth asking about.
Transcranial Direct Current Stimulation (tDCS)
This is a non-invasive brain stimulation technique that uses a low electrical current applied to the scalp to modulate neural activity. For fibromyalgia, the target is typically the motor cortex or the dorsolateral prefrontal cortex â areas involved in pain processing.
A 2022 meta-analysis in The Journal of Pain found that tDCS produced significant reductions in pain intensity in fibromyalgia patients, with effects lasting several weeks after treatment. Some clinics now offer tDCS as part of a multimodal pain management program, and home-use devices are becoming available under medical supervision.
The appeal of tDCS is that it directly targets the central sensitization that drives fibromyalgia pain, rather than masking symptoms with medication.
Psilocybin-Assisted Therapy
This is still in the early research stages, but the preliminary findings are remarkable. Psilocybin â the active compound in certain mushrooms â appears to “reset” pain processing networks in the brain. A 2024 pilot study at Imperial College London found that a single guided psilocybin session produced significant pain reduction in fibromyalgia patients that persisted for up to 12 weeks.
This is not a treatment you can access easily yet. Clinical trials are ongoing, and legal access is limited to specific research settings. But it represents a fundamentally different approach to fibromyalgia â one that targets the neurological root rather than the symptoms.
Vagus Nerve Stimulation
The vagus nerve plays a central role in regulating inflammation and pain perception. Non-invasive vagus nerve stimulation (nVNS) devices â which deliver mild electrical pulses to the vagus nerve through the skin of the neck or ear â are showing promise for fibromyalgia.
A 2023 study in Pain Medicine found that daily nVNS use over eight weeks reduced widespread pain intensity and improved sleep quality in fibromyalgia patients. Devices like gammaCore are already FDA-cleared for migraine and cluster headache, and research for fibromyalgia applications is expanding.
Acupressure for Fibromyalgia
This is where I can speak from years of direct experience, both personal and from the hundreds of people with fibromyalgia who have shared their results with me. Acupressure is one of the most effective non-pharmaceutical treatments for fibromyalgia, and the research backs this up.
A 2020 randomized controlled trial published in The Journal of Pain found that self-administered acupressure performed daily for six weeks produced significant reductions in pain, fatigue, and sleep disturbance in fibromyalgia patients. The improvements persisted for weeks after the treatment period ended.
The reason acupressure works so well for fibromyalgia comes down to how it interacts with the nervous system. Sustained pressure on specific points triggers the release of endorphins and enkephalins â your body’s natural painkillers. It activates the parasympathetic nervous system, which counters the chronic sympathetic overdrive that many fibromyalgia patients experience. And it increases blood flow to painful areas, which helps reduce the local inflammation and muscle tension that compound the central pain.
Key Acupressure Points for Fibromyalgia
The points I recommend most often for fibromyalgia relief include Large Intestine 4 (He Gu), located in the fleshy web between the thumb and index finger. This is the master point for pain anywhere in the body and is particularly effective for the widespread aching that defines fibromyalgia.
Liver 3 (Tai Chong), on the top of the foot between the first and second toes, works in combination with LI 4 in what traditional Chinese medicine calls the “Four Gates.” Together, these four points (both hands and both feet) promote full-body energy flow and pain relief.
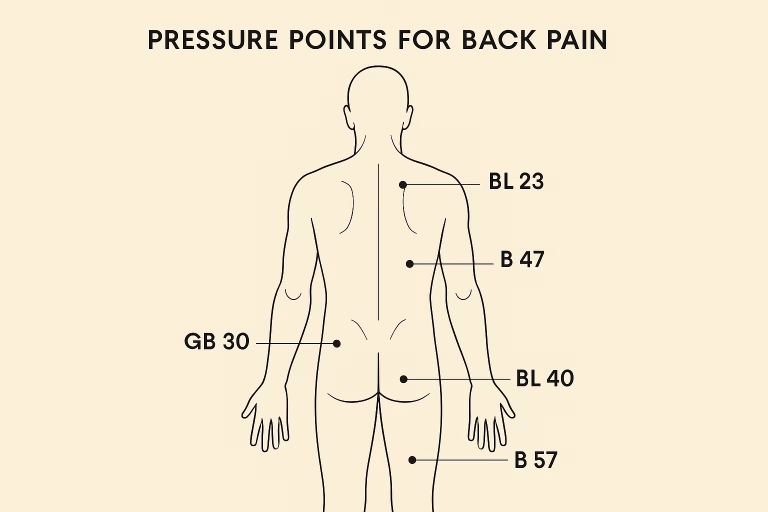
Gallbladder 20 (Feng Chi), at the base of the skull, targets the headaches and neck tension that accompany fibromyalgia for many people. Spleen 6 (San Yin Jiao), above the inner ankle, addresses fatigue and sleep disturbances. And Bladder 23 (Kidney Shu), on either side of the lower spine, targets the deep back pain that is one of the most common fibromyalgia complaints.
Press each point firmly for 60 to 90 seconds, breathing deeply. For a full-body treatment, work through all these points in sequence â it takes about 10 minutes and the cumulative effect is significant.
Using an Acupressure Mat for Fibromyalgia
For people with fibromyalgia, an acupressure mat offers something that manual point pressing cannot â simultaneous stimulation of hundreds of pressure points across the entire back. This is particularly valuable because fibromyalgia pain is widespread rather than localized.
I have been using my Pranamat daily since 2017, and it was specifically the fibromyalgia-related tension and pain I was hearing about from readers that led me to investigate acupressure mats in the first place. The mat stimulates blood flow across the entire back, releases endorphins systemically, and activates the parasympathetic nervous system â all of which directly address the mechanisms driving fibromyalgia pain.
The key for fibromyalgia patients is starting slowly. Your nervous system is already sensitized, so the initial sensation can be more intense than it would be for someone without fibromyalgia. Start with a thin t-shirt between you and the mat, and limit your first few sessions to 10 minutes. Most people can work up to 20 minutes on bare skin within two to three weeks, and this is where the real benefits accumulate.
The consistency matters more than the duration. Fifteen minutes every day is more effective than 30 minutes three times a week. Your nervous system needs the daily signal to start recalibrating its pain response.
Exercise and Movement Therapies
Exercise is arguably the single most evidence-supported treatment for fibromyalgia, yet it is also the most challenging to implement. When everything hurts, the last thing you want to do is move. But the right kind of movement, at the right intensity, can fundamentally change your pain levels.
Water-Based Exercise
Pool-based exercise is the gold standard starting point for fibromyalgia. The buoyancy reduces joint loading by up to 90%, the warm water relaxes muscles and reduces pain sensitivity, and the hydrostatic pressure provides gentle compression that can feel soothing.
A 2019 Cochrane review confirmed that aquatic exercise produces moderate improvements in pain, physical function, and stiffness in fibromyalgia patients. The improvements were comparable to land-based exercise, but adherence was significantly higher â because it feels better while you are doing it.
If you have access to a warm pool (ideally 33-36 degrees Celsius), start with 20 minutes of gentle movement â walking in the water, gentle arm circles, leg lifts. Build gradually over weeks. The goal is not cardiovascular fitness; it is teaching your nervous system that movement is safe.
Tai Chi and Qigong
Tai chi has emerged as one of the most effective movement therapies for fibromyalgia. A landmark 2018 study in the British Medical Journal found that tai chi was at least as effective as aerobic exercise â the current gold-standard recommendation â for reducing fibromyalgia symptoms over 24 weeks. Some participants saw even greater benefits from tai chi.
The slow, deliberate movements combined with deep breathing and meditative focus address multiple fibromyalgia mechanisms simultaneously: they reduce stress, improve proprioception, gently challenge the musculoskeletal system, and calm the overactive nervous system.
Qigong, a related practice, has shown similar benefits. Both are available through community classes, online programs, and many physical therapy practices.
Yoga for Fibromyalgia
Yoga can be excellent for fibromyalgia, but the type matters enormously. Gentle restorative yoga and yoga nidra (a form of guided relaxation) show the strongest evidence. Power yoga, hot yoga, and vigorous vinyasa flows can trigger flare-ups.
A 2021 systematic review in Pain Research and Management found that yoga programs lasting at least eight weeks produced significant improvements in pain, fatigue, mood, and physical function in fibromyalgia patients. The key is consistency and gentleness â a 20-minute daily practice is more beneficial than an intense 90-minute weekly class.
Sleep Optimization
Poor sleep and fibromyalgia create a vicious cycle. The pain disrupts sleep, and poor sleep amplifies pain sensitivity. Breaking this cycle is one of the most impactful things you can do.
Sleep hygiene basics matter, but for fibromyalgia they need to be more rigorous than for the general population. Keep your bedroom cool (18-20 degrees Celsius), completely dark, and free of screens for at least 30 minutes before bed. Maintain a consistent sleep and wake time, even on weekends.
Cognitive behavioral therapy for insomnia (CBT-I) has strong evidence specifically for fibromyalgia-related sleep disturbance. It is more effective than sleeping pills for long-term improvement and does not carry the side effect burden. Many therapists now offer CBT-I online.
An evening acupressure mat session can be a powerful sleep aid. Lying on my Pranamat for 20 minutes before bed activates the parasympathetic nervous system â the “rest and digest” branch â which helps your body transition into sleep mode. Many fibromyalgia patients tell me this is the single biggest change they noticed from daily mat use: they sleep better.
Stress and Nervous System Regulation
Fibromyalgia is, at its core, a disorder of nervous system regulation. The autonomic nervous system is stuck in a state of hypervigilance â the sympathetic (“fight or flight”) branch is chronically overactive, and the parasympathetic (“rest and digest”) branch is underactive. Any effective treatment plan must address this imbalance.
Daily practices that activate the parasympathetic nervous system include diaphragmatic breathing (slow, deep belly breaths with extended exhales), meditation and mindfulness, time in nature, warm baths, and acupressure. The key is daily consistency. Five minutes of deep breathing every day is more effective than an hour-long meditation once a week.
Heart rate variability (HRV) biofeedback is a newer approach gaining traction for fibromyalgia. By training you to increase the variability between heartbeats â a marker of parasympathetic activity â it helps shift your nervous system toward a calmer baseline. Several HRV training apps and devices are now available for home use.
Nutrition and Supplements
While no single diet cures fibromyalgia, what you eat can significantly influence your symptom severity.
An anti-inflammatory diet â rich in fatty fish, vegetables, fruits, nuts, and olive oil while minimizing processed foods, sugar, and alcohol â provides the foundation. A 2021 study in Nutrients found that fibromyalgia patients who followed an anti-inflammatory diet for 12 weeks reported significant improvements in pain and fatigue.
Specific supplements with evidence for fibromyalgia include vitamin D (deficiency is common in fibromyalgia and correction often improves symptoms), magnesium (which supports muscle relaxation and sleep), coenzyme Q10 (which may reduce fatigue), and omega-3 fatty acids (which help modulate inflammation). As with any supplement, discuss these with your doctor, particularly if you are taking medications.
Building Your Treatment Plan
The most effective approach to fibromyalgia is multimodal â combining several strategies that target different mechanisms. No single treatment is likely to be enough on its own, but the right combination can be transformative.
A practical starting point combines daily acupressure (either manual point work or an acupressure mat session of 15-20 minutes), gentle movement three to five times per week (starting with whatever you can tolerate â even 10 minutes of walking counts), sleep optimization including evening relaxation practices, an anti-inflammatory nutrition focus, and daily stress management through breathing or meditation.
Start with one or two changes and build gradually. Adding everything at once is overwhelming and unsustainable, especially when you are already dealing with fatigue and pain. Give each new practice two to three weeks before evaluating its impact â your nervous system needs time to respond.
When to Seek Specialized Care
While self-management strategies are powerful, some situations warrant specialized medical attention. Consider seeing a fibromyalgia specialist if your symptoms are significantly worsening despite consistent self-care, your current medications are causing problematic side effects, you are developing new symptoms that do not fit your typical fibromyalgia pattern, your pain is preventing you from basic daily activities, or you are interested in newer treatments like LDN or neuromodulation that require medical supervision.
A rheumatologist or pain management specialist with specific experience in fibromyalgia can offer the most targeted care. Do not settle for a provider who dismisses fibromyalgia as “not real” â you deserve better than that.
The Bottom Line
Fibromyalgia treatment in 2026 looks very different from even five years ago. We now understand that this is a disorder of central pain processing, not imagined pain or simple muscle soreness. And with that understanding comes better treatments â from low-dose naltrexone and neuromodulation to acupressure, movement therapies, and nervous system regulation techniques.
The patients who do best are the ones who build a comprehensive, daily approach rather than relying on any single intervention. An acupressure mat session plus gentle movement plus good sleep plus anti-inflammatory nutrition creates a foundation that changes the trajectory of the condition.
Your nervous system learned to amplify pain. With the right inputs, consistently applied, it can learn to turn the volume back down. That is not false hope â it is what the evidence shows.
Frequently Asked Questions
What is the most promising new treatment for fibromyalgia?
Low-dose naltrexone (LDN) is currently the most promising emerging medical treatment. Studies show an average 30% reduction in pain scores, with minimal side effects. It works by reducing neuroinflammation through microglial cell modulation. While not yet FDA-approved for fibromyalgia specifically, it is available as an off-label prescription. Ask your doctor about it if your current treatment is not providing adequate relief.
Does acupressure help fibromyalgia?
Yes. Research shows that self-administered acupressure reduces pain, fatigue, and sleep disturbance in fibromyalgia patients. Acupressure works by triggering endorphin release, activating the parasympathetic nervous system, and increasing blood flow to painful areas. An acupressure mat like the Pranamat provides widespread stimulation that is especially suited to the diffuse pain pattern of fibromyalgia. I have been using acupressure since 2017 and it remains one of the most effective tools I recommend.
What is the best exercise for fibromyalgia?
Water-based exercise is the best starting point because the buoyancy and warmth reduce pain during movement. Tai chi is also highly effective â a major BMJ study found it was at least as effective as aerobic exercise for fibromyalgia. Gentle yoga, walking, and swimming are also beneficial. The key is starting gently, building gradually, and prioritizing consistency over intensity.
Can fibromyalgia go into remission?
While fibromyalgia is generally considered a chronic condition, many people achieve significant symptom reduction â sometimes to the point where it no longer significantly impacts daily life. This typically requires a comprehensive approach combining movement, sleep optimization, stress management, and pain relief strategies like acupressure. Complete remission is less common but does occur, particularly with early intervention.
What foods should I avoid with fibromyalgia?
Processed foods, refined sugars, excessive alcohol, and artificial additives tend to worsen fibromyalgia symptoms by promoting inflammation. Some people also find that gluten, dairy, or nightshade vegetables trigger flare-ups, though this varies individually. An anti-inflammatory diet rich in fatty fish, vegetables, nuts, and olive oil provides the strongest evidence base for symptom improvement.
How long does it take for fibromyalgia treatments to work?
Most non-pharmaceutical treatments take four to eight weeks of consistent daily practice to produce noticeable improvements. Acupressure mat use often provides immediate relaxation, but the cumulative pain-reducing effects build over several weeks. Medications like LDN typically require two to three months to reach full effect. Exercise programs generally show significant results within eight to twelve weeks.
Is fibromyalgia a real condition?
Absolutely. Fibromyalgia is a well-documented disorder of central pain processing with identifiable changes in brain structure and function. Neuroimaging studies show that fibromyalgia patients have altered pain processing in the brain and spinal cord. It is recognized by the World Health Organization, the American College of Rheumatology, and every major medical organization. If a healthcare provider dismisses your symptoms, find one who takes them seriously.
Related Reading
- Acupressure Mats and Fibromyalgia
- Acupressure Mat Benefits
- Pressure Points for Back Pain
- Pressure Points for Stress
- How to Use Acupressure Mat for Lower Back Pain
Free Mobile App
Find Pressure Points on the Go
Interactive 3D body map with 100+ acupressure points, step-by-step guides, and personalized routines.
Download Free App →